What is a Total Knee Replacement?
A total knee replacement (TKR) is an operation that resurfaces the worn-out ends of the knee joint with smooth, durable artificial components. It is one of the most common and effective procedures for advanced knee arthritis, providing long-lasting pain relief and improved function.
Treatment for a total knee replacement includes preparation before surgery, the operation itself, and post-operative rehabilitation, all of which are explained here.
Why consider a total knee replacement?
A knee replacement is offered when:
- Pain significantly limits daily activities
- Physiotherapy, injections or medications no longer provide relief
- Sleep, walking distance or ability to work are affected
- The knee becomes stiff, unstable or bowed
- X-rays show moderate to severe arthritis
The goal of treatment is simple: less pain, improved mobility, better quality of life.
Pre-operative Treatments & Preparation
Before surgery, several steps help ensure you are safe, prepared, and able to recover well.
→ Physiotherapy
→ Strengthening exercises
→ Weight optimisation (if appropriate)
→ Walking aids (stick/crutches) if needed
These measures help maintain strength and stability ahead of surgery.
→ Review your medical history
→ Check blood tests, ECG and other investigations
→ Discuss anaesthetic options (spinal, general, or combined)
→ Ensure you are medically optimised for surgery
Exercises may include:
→ Straight leg raises
→ Knee extension and flexion
→ Gluteal and core strengthening
Treatment During Surgery: What Happens in a Total Knee Replacement?
The operation normally takes 60–90 minutes and is performed through a carefully planned incision at the front of the knee.
→ The end of the thigh bone (femur)
→ The top of the shin bone (tibia)
In many cases, the worn surface on the back of the kneecap is also resurfaced.
→ The medial compartment
→ The lateral compartment
→ The patellofemoral joint
Because the entire joint is replaced, damaged cartilage and bone are fully addressed, providing reliable pain relief in advanced arthritis.
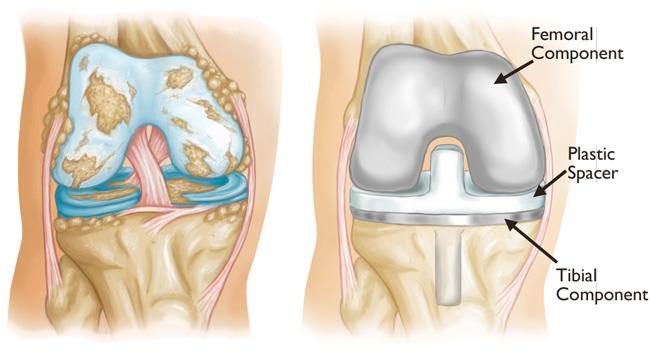
→ Femoral component – a shaped metal implant covering the end of the thigh bone
→ Tibial component – a metal baseplate fixed to the top of the shin bone
→ Polyethylene insert – a durable plastic spacer that allows smooth movement
→ Patellar component (if required) – a plastic button resurfacing the kneecap
Most TKRs are cemented, providing immediate fixation and long-term durability.
→ Smooth, stable motion
→ Balanced ligaments
→ Correct leg alignment
Implant positioning and soft tissue balance are fine-tuned at this stage to optimise function and longevity.
Removing the Damaged Surfaces
01
The worn cartilage and arthritic bone at the end of the thigh bone (femur) and shin bone (tibia) are removed.
Preparing the Bone
04
The bone surfaces are shaped precisely to accept the implants, ensuring accurate alignment and stability.
Inserting Implants
02
- A typical knee replacement consists of:
- Femoral component – metal surface for the end of the thigh bone
- Tibial component – metal tray fixed to the shin bone
- Plastic insert (polyethylene) – a smooth, durable bearing between the components
- Patellar button (optional) – resurfacing the kneecap depending on arthritis severity
- Implants may be: Cemented (most common) Uncemented (select cases)
- Your surgeon will choose the most appropriate implant based on bone quality, age and activity level.
Checking Alignment, Stability and Movement
03
- The knee is tested to ensure:
- Smooth bending and straightening
- Correct ligament balance
- Proper alignment of the leg
Closing the Wound
05
Layers are closed—often with dissolvable sutures—and a dressing is applied.
total knee replacement post operative recovery
Recovery is vital to achieving a successful outcome. Most patients stand and walk on the day of surgery or the following morning.
Pain Management
- Modern multimodal techniques reduce pain and accelerate recovery, including:
- Spinal anaesthetic with light sedation
- Local anaesthetic around the knee
- Oral pain medications
- Ice therapy
- Most patients require only mild analgesics after the first week.
Early Mobilisation
- A physiotherapist will help you:
- Stand and walk safely
- Use crutches or walking aids
- Begin knee bending and straightening exercises
- Early mobilisation reduces stiffness and lowers the risk of blood clots.
Physiotherapy and Rehabilitation
- Rehabilitation focuses on:
- Stand and walk safely
- Quadriceps strengthening
- Gait training
- Balance and functional exercises
- Typical recovery milestones:
- Driving: ~6 weeks
- Desk-based work: 2–4 weeks
- Walking unaided: 4–6 weeks
- Golf/cycling: 8–12 weeks
- Full activity: 3–6 months
Long-term Treatment After Knee Replacement
Continuing Strength & Mobility
- Recommended low-impact activities include:
- Walking
- Swimming
- Cycling
- Pilates or yoga
- These maintain joint movement and reduce stiffness.
Protecting Your New Knee
- Avoid high-impact activities early such as:
- Long-distance running
- Repetitive jumping sports
- Heavy manual labour with high knee load
- Gradually build up with physio guidance
Ongoing Review
- Follow-up appointments allow monitoring of:
- Wound healing
- Knee movement and strength
- X-rays to check the implant
- Most modern knee replacements last 15–20 years or more, depending on activity levels.
Risks and Complications
All operations carry risks, although knee replacement is a very safe procedure. Potential complications include:
- Infection
- Blood clots
- Stiffness
- Persistent pain
- Fracture during surgery
- Nerve or vessel injury (rare)
- Implant wear or loosening over time
You will have the opportunity to discuss all risks and benefits in detail.


